Ivcd with st elevation4/12/2023  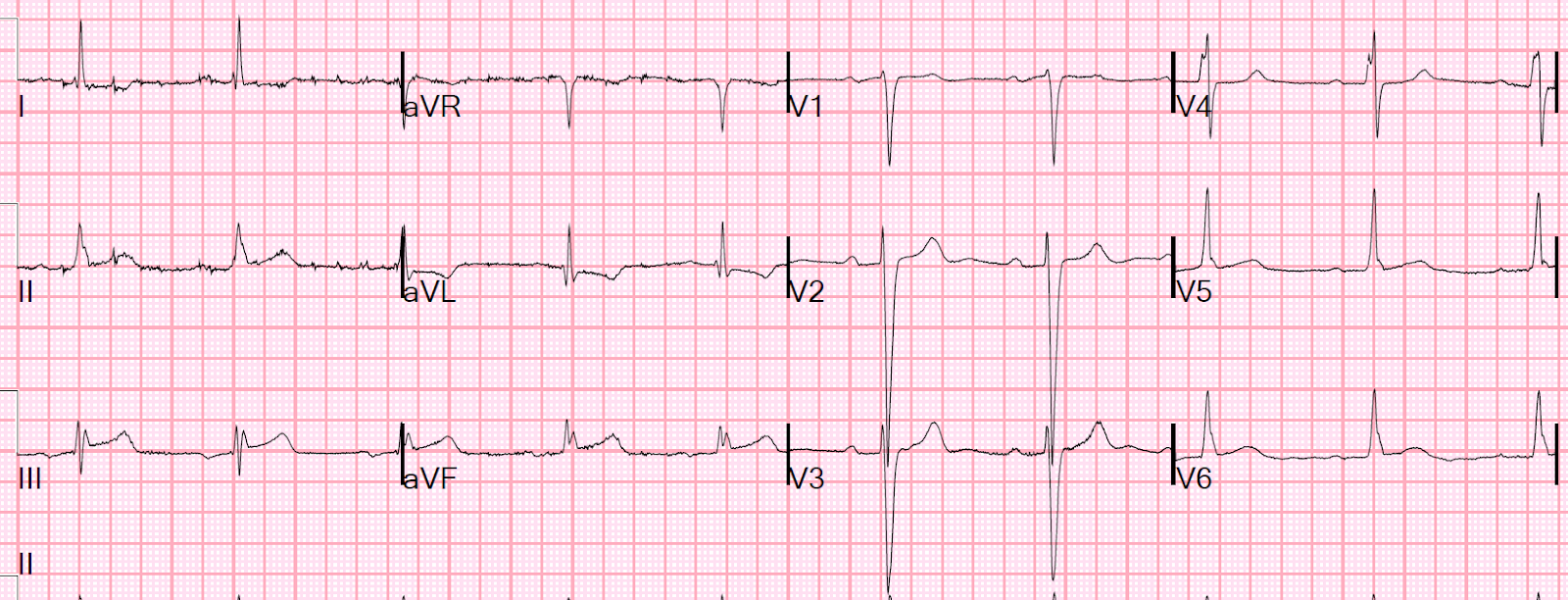
Concave upwards ST elevation in most leads except aVR.ST elevation during exercise testing suggests extremely tight coronary artery stenosis or spasm (transmural ischemia).ST elevation may also be seen as a manifestation of Prinzmetal's (variant) angina (coronary artery spasm).Persistent ST elevation after acute MI suggests ventricular aneurysm.Acute transmural injury - as in this acute anterior MI.Ischemic Heart Disease (usually convex upwards, or straightened) Neurogenic effects (e.g., subarrachnoid hemorrhage causing long QT)ĭifferential Diagnosis of ST Segment Elevation Normal Variant "Early Repolarization" (usually concave upwards, ending with symmetrical, large, upright T waves)Įxample #1: "Early Repolarization": note high take off of the ST segment in leads V4-6 the ST elevation in V2-3 is generally seen in most normal ECG's the ST elevation in V2-6 is concave upwards, another characteristic of this normal variant.Ischemia, infarction, inflammation, etc.Electrolyte abnormalities (e.g., hypokalemia).Drug effects (e.g., digoxin, quinidine, etc)."Primary" ST-T Wave Abnormalities (ST-T wave changes that are independent of changes in ventricular activation and that may be the result of global or segmental pathologic processes that affect ventricular repolarization): ST-T changes in PVCs, ventricular arrhythmias, and ventricular paced beats. 
ST-T changes seen in bundle branch blocks (generally the ST-T polarity is opposite to the major or terminal deflection of the QRS)."Secondary" ST-T Wave changes (these are normal ST-T wave changes solely due to alterations in the sequence of ventricular activation): Ventricular conduction abnormalities and rhythms originating in the ventricles.Atrial repolarization (e.g., at fast heart rates the atrial T wave may pull down the beginning of the ST segment).Metabolic factors (e.g., hypoglycemia, hyperventilation).Neurogenic factors (e.g., stroke, hemorrhage, trauma, tumor, etc.).Electrolyte abnormalities of potassium, magnesium, calcium.Drugs (e.g., digoxin, quinidine, tricyclics, and many others).Intrinsic myocardial disease (e.g., myocarditis, ischemia, infarction, infiltrative or myopathic processes).Patient to ascertain the importance of the ECG findings.įactors affecting the ST-T and U wave configuration include: Thisĭoes not mean that the ECG changes are unimportant! It is the responsibility of the clinician providing care for the Thus the term, nonspecific ST-T waveĪbnormalities, is frequently used when the clinical data are not available to correlate with the ECG findings. In which the ECG changes are found than by the particular changes themselves. General Introduction to ST, T, and U wave abnormalitiesīasic Concept: the specificity of ST-T and U wave abnormalities is provided more by the clinical circumstances General Introduction to ST-T and U Wave Abnormalities.Frequently an IVCD will look like a left bundle branch block in lead V1 with an rS complex or monomorphic S wave, and it appears like a right bundle branch block in leads I and V6 with a broad, slurred S wave.ĭecreased amplitude of the P waves, an increase in the PR interval, and bradycardia in the form of AV blocks occur as the potassium level exceeds 7.0.Ībsence of the P waves and, eventually, a "sine wave" pattern (see below), which is frequently a fatal rhythm. This usually requires a potassium level of 6.5 or greater and frequently appears as in "intraventricular conduction delay" or IVCD, which is characterized by a widened QRS complex of > 120 ms that does not meet the criteria for a left or right bundle branch block. Peaked T waves best seen in the precordial leads, shortened QT interval and, sometimes, ST segment depression. From earliest to latest, the ECG findings include: The ECG findings of hyperkalemia change as the potassium level increases. 
0 Comments
Leave a Reply.AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
